By Jordan Stachel
Lyme disease is a tick-borne infection thought to affect between 300,000 and 476,000 Americans each year, according to the U.S. Centers for Disease Control and Prevention. While incidence rates have seemed to increase over the past few years, this range is likely overestimated, as many people are presumptively treated for Lyme disease.
What Are the Symptoms and Early Signs of Lyme Disease?
Lyme disease can present with many symptoms that vary among individuals, making an appropriate diagnosis tricky.
Early signs and symptoms of Lyme disease may include:
- Fever.
- Chills.
- Headache.
- Sensitivity to light.
- Fatigue.
- Muscle aches.
- Swollen lymph nodes.
- An erythema migrans (EM) rash that may appear in a “bullseye” shape. Contrary to popular belief, the bullseye is not as typical as other manifestations of the rash. It is more typically uniform in color, round (like a spider bite), and/or bluish in color.
If Lyme disease goes untreated, further signs and symptoms may develop, including:
- More severe headaches.
- Facial palsy (nerve weakness on one side of the face).
- Arthritis.
- Pain in the bones.
- Heart palpitations or an irregular heartbeat.
- Dizziness.
- Nerve pain.
- Inflammation in the brain or spinal cord.
- Numbness in the hands or feet.
The good news is that most people do not die from Lyme disease unless complications begin to have a systemic and severe effect on the body.
What Causes Lyme Disease?
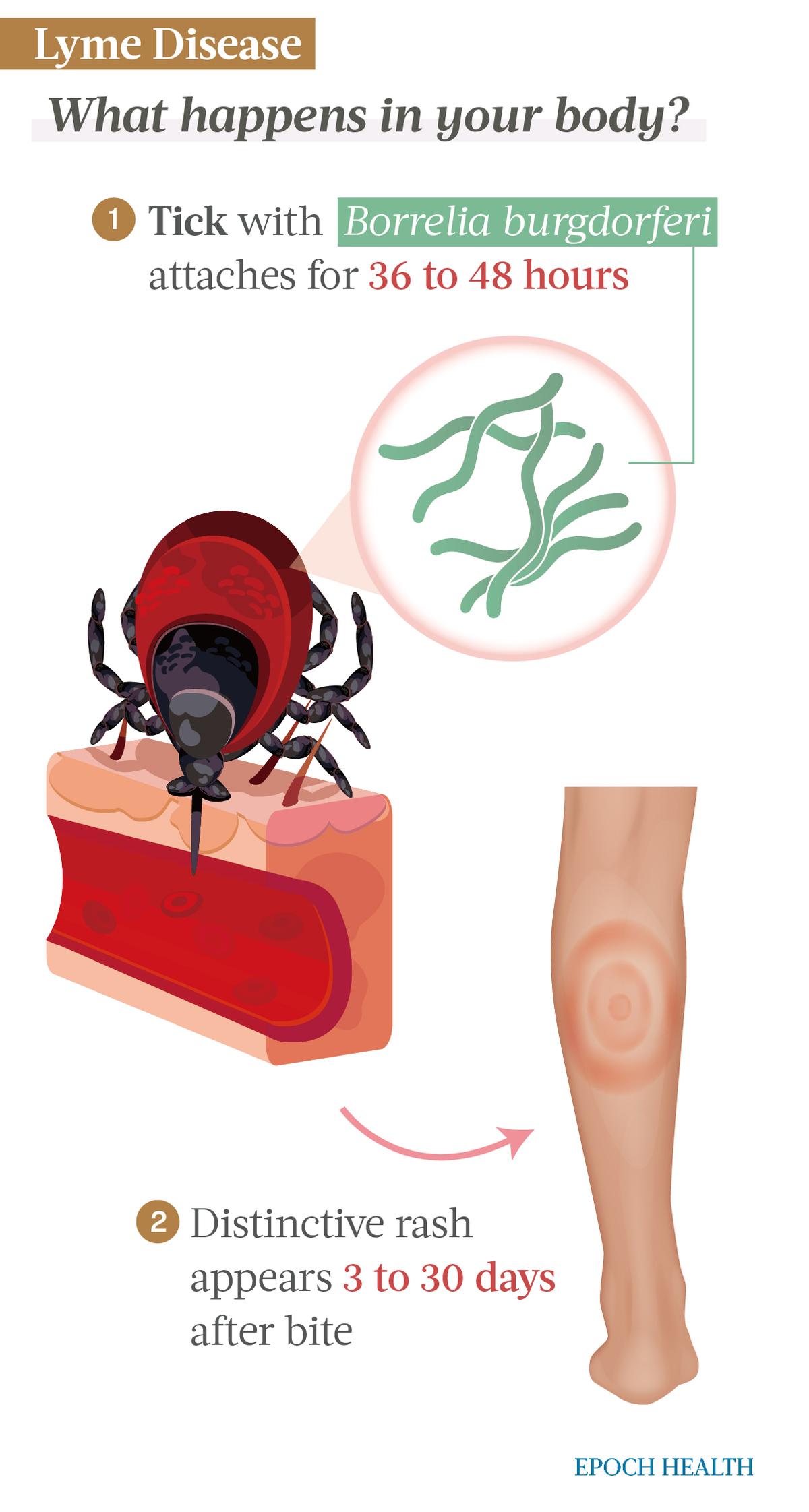
Lyme disease is caused by the bacteria Borrelia burgdorferi and Borrelia mayonii, transmitted to humans via tick bites. Typically, black-legged ticks, also known as deer ticks, are the type of ticks that transmit infection, and these have a two-to-three-year life cycle.
For an infection to occur, a tick typically must be attached to a person’s skin for 36 to 48 hours before bacteria begin to be transmitted. If ticks are found before this window of time, there is a chance that Lyme disease transmission can be avoided.
What Are the Stages of Lyme Disease?
The different stages of Lyme disease are as follows:
- Stage 1 (early localized): Lyme disease is localized. Patients may present with a rash, known as erythema migrans, on or near the bite site and/or with a low-grade fever. This initial stage typically occurs within the first month following a tick bite. Many people may not exhibit any signs or symptoms in stage 1.
- Stage 2 (early disseminated): People may experience more symptoms in this stage, including fatigue, dizziness, and cardiac-based symptoms. Stage 2 Lyme disease typically develops between weeks three and 12 after an infection. This is the stage in which Lyme disease is more disseminated, or has spread, throughout the body.
- Stage 3 (late persistent): This stage typically develops months to years after an infection. During this stage, neurological symptoms, arthritis (especially in the knees), and heart rhythm complications may be common. It is vital to seek medical treatment if experiencing these symptoms.
It is also important to note that Lyme disease can develop alongside other tick-based coinfections, as ticks may be infected with more than one disease-causing microbe when they infect a person. Some of these coinfections include:
- Babesia: This malaria-like parasite infects red blood cells and may induce similar symptoms to Lyme disease. This is typically treated with antimalarial drugs and antibiotics.
- Bartonella: These bacteria infect red blood cells and may induce a streaked rash similar to stretch marks. Bartonella also must be treated with a combination of antibiotics.
- Rickettsia: These bacteria can cause fever, severe headache, rash, and muscle pain and weaken the body’s blood vessels. The condition is typically treated with oral medications and/or intravenous antibiotics. The most common rickettsial infection in the United States is Rocky Mountain spotted fever.
Who Is More Likely to Develop Lyme Disease?
Because Lyme disease is preventable, one must be aware of the risk factors that put an individual at a higher risk for developing it.
Most of the time, people have a higher risk of being infected during the spring through fall, but it’s possible to be infected if the weather stays above freezing.
Some of these factors include:
- Living in certain states and regions in the United States, including the Northeast, mid-Atlantic states, Wisconsin, Minnesota, and northern California.
- Living in suburban or more rural areas, as areas with more vegetation increase one’s likelihood of encountering ticks.
- Working outside.
- Outdoor activities like hiking, hunting, or gardening in higher transmission areas.
- Having pets that may bring ticks in from outside.
How Is Lyme Disease Diagnosed?
If you have a rash similar to the telling bullseye rash or symptoms similar to those of Lyme disease, your doctor may perform the following tests.
- Blood tests: Diagnosing Lyme disease usually is a two-step process. Blood tests look for bacteria buildup in the body that causes Lyme disease. The first recommended blood test is an enzyme-linked immunoassay (ELISA) test that tests for antibodies in your blood formed to fight Lyme disease. It can return with false negatives if performed too close to the time of the suspected bite, as it takes a few weeks for the antibodies to develop. Two options are available if a second test is needed: a second ELISA test or a Western blot, which is sometimes preferred for later-stage Lyme disease.
- Cerebrospinal fluid (CSF) test: A CSF test may be performed if Lyme disease has been thought to affect your nervous system and/or if blood test results come back inconclusive.
- Polymerase chain reaction (PCR) tests: PCR tests can detect the genetic material (DNA) of the Lyme bacteria. These tests are typically only accurate if a person has an active infection.
If a diagnosis of Lyme disease is confirmed, obtaining a comprehensive action plan from a team of qualified health care providers is advised to optimize outcomes.
What Are the Complications of Lyme Disease?
Lyme disease can lead to several complications, with the potential for all bodily systems to be affected depending on the progression and manifestation of the condition.
Some of the most common complications of later-stage Lyme disease include:
- Persistent fatigue.
- Inflammation and arthritis: A person may experience joint pain and/or swelling in the knees, elbows, shoulders, wrists, ankles, or hips. This can usually be treated with antibiotics and/or nonsteroidal anti-inflammatory drugs (NSAIDs).
- Nerve damage: Nerve damage may result in weakness in several areas of the body and may also cause pain, numbness, and/or tingling.
- Neurological complications: Neurological complications, also known as neuroborreliosis, like confusion, loss of memory, difficulty concentrating, or other speech problems are possible.
- Post-Lyme disease syndrome: This condition can occur after Lyme disease has been treated with antibiotics. If this happens, people may experience persistent fatigue, aching muscles, trouble with cognition, and headaches. This syndrome is often diagnosed if people are still experiencing symptoms six months post-treatment.
- Lyme carditis: This rare complication occurs in only about 1 percent of cases but can be a serious complication of Lyme disease.
What Are the Treatments for Lyme Disease?
The treatments for Lyme disease will vary based on the condition’s advancement and what your team of health care providers deems most appropriate. Common treatments usually involve antibiotics but may include a combination of more naturopathic treatment modalities.
Antibiotics
Oral antibiotics such as doxycycline, amoxicillin, and cefuroxime are used to help fight Lyme disease. Additional medication may be prescribed to manage Lyme disease symptoms, such as those that target pain, inflammation, or cognition.
How Does Mindset Affect Lyme Disease?
Because Lyme disease has a clear physical cause, mindset does not directly impact whether or not you develop it. However, how you mentally cope with a diagnosis can affect your quality of life.
Research indicates that Lyme disease can affect an individual’s quality of life, sleep quality, attention span, frequency of depressive symptoms, memory performance, and ability to thrive in one’s career. In all of these areas, generally, people living with Lyme disease were shown to have worse outcomes when compared to the control groups. This is thought to be due to the mental and physical toll that Lyme disease can take on a person.
What’s promising is that some research indicates that positive mental health practices can significantly improve perceived quality of life and symptom recurrence for those with Lyme disease.
To begin, it is helpful to monitor symptoms and perceived quality of life by keeping a symptom journal to share with a health care provider. This can help begin to track symptom recurrence and identify patterns. Monitoring things like changes in appetite, energy, and mood are all helpful indicators of overall mental health status that can give a health care provider more insight into how to provide personalized guidance and suggestions.
In addition, taking a proactive approach by engaging in stress-reducing, meditative practices can be helpful for those living with Lyme disease. Some research indicates that the practice of kundalini yoga may aid people in mitigating common symptoms. Patients practicing this type of yoga showed improvement in multisystem symptom relief, cognition, and fatigue.
While more research is needed in examining behavioral interventions like yoga practice to help improve mindset and, secondarily, symptoms for those with Lyme disease, this encouraging study indicates the robust correlation between the mind and body.
What Are the Natural Approaches to Lyme Disease?
While traditional treatment for Lyme disease is centered around antibiotics and other medications, natural approaches may aid in managing symptoms for those living with Lyme.
Some laboratory cell culture research has attempted to uncover the mechanism by which essential oils may help symptom management. Many theorize that the antimicrobial properties of these oils may help control the growth of the bacterial pathogen. While further research is needed on these specific combinations of essential oils, there is likely no downside to someone with Lyme disease diffusing them in their environments. Within this particular study of cultures, the following oils showed effectiveness in activity against the bacteria, with the active compound in oregano being the most effective:
- Bandit.
- Oregano.
- Clove bud.
- Geranium bourbon.
- Cinnamon bark.
In addition, following an anti-inflammatory diet with the inclusion of a variety of foods can help mitigate symptoms. Limiting processed foods, refined carbs, sugars, and inflammatory seed oils may help those living with Lyme disease experience less inflammation, improving symptoms and quality of life.
Because the majority of the immune system resides in the gut, and the gut is where nutrients are absorbed, the health of your microbiome is vital. Including anti-inflammatory, fiber-rich foods can help feed the good gut bacteria within the gastrointestinal system and thus improve overall immunity. Including foods like fatty fish, vegetables, healthy fats, fruits, and whole grains is a great jumping-off point for building an anti-inflammatory regimen. For personalized guidance, it is always advised to consult a qualified health care provider.
Supplementing with anti-inflammatory nutrients and vitamins may also improve symptoms in people with Lyme disease. A high-quality multivitamin that includes vitamin D, vitamin A, and zinc may be helpful. A high-quality multivitamin might also bridge nutrient gaps and bolster an individual’s immune system. As always, consulting your doctor or qualified health care practitioner before adding any new supplement to your routine is advised.
Some research points toward hyperbaric oxygen therapy as a natural treatment for chronic Lyme disease. During this treatment, oxygen is inhaled within a chamber pressurized with pressure greater than at sea level. This is thought to potentially help inhibit bacterial growth by allowing the cells to improve their ability to kill bacteria more effectively.
While there is some anecdotal evidence of people with Lyme disease benefiting from additional natural treatment approaches like saunas, steam rooms, ultraviolet light, and bee venom, there is insufficient clinical research to support these claims.
In combination with antibiotics, or if symptoms persist after someone has been treated with antibiotics, additional approaches may be taken to alleviate symptoms and improve quality of life. Some of these include:
- Stress-reducing techniques to help manage pain (therapy, meditation, etc.).
- Mind-body practices like qigong to help improve posture, movement, and breathing techniques.
- Acupuncture to aid in reducing fatigue.
- Cognitive behavioral therapy (CBT) and relaxation techniques to help promote a better night’s sleep.
- Lemon balm and/or melatonin supplements to aid in sleep.
- Online brain training exercises to aid in enhancing concentration and/or working memory for those experiencing cognitive symptoms.
How Can I Prevent Lyme Disease?
Some of the best ways to reduce your risk of developing Lyme disease include:
- Remaining aware of environmental exposure: In areas with tall grass or overgrown brush, wear long pants and sleeves to mitigate exposure. In addition, staying in the middle of trails while hiking, wearing insect repellent, and showering immediately after returning from an outdoor activity can help. Also, tuck pant legs into socks when walking through tall grass.
- Self-examination: If you think there is a chance that you or a family member could be exposed to ticks, it is advised to do self-examinations each time you come back from an outdoor activity. If you find a tick, it is important to properly remove it immediately, ensuring you pluck it by the head and not by its exposed backside.
- Creating a tick-free zone: Creating a tick-safe zone is advised if you live or work in a high-risk area. Using chemical control agents and keeping deer away are helpful tips for reducing risk.
Medically reviewed by Beverly Timerding, MD.






