By Marisa Schultz | Fox News
Already overwhelmed by the scarcity of protective gear and the dangers of treating a highly contagious virus, many American doctors on the front lines of the COVID-19 pandemic have been dealt another punch in the gut.
ShadeMaker Shades – Architectural Patio Shade
Shop ShadeMaker from PatioProductsUSA. Shop with Confidence & Call Experts Now
In recent days and weeks, doctors across the country have been notified that their pay will be slashed during the height of the coronavirus health emergency.
“Honestly, my life is hell right now,” said one emergency medicine doctor in Los Angeles who just learned her pay will be cut at least 25 percent.
The doctor who treats COVID-19 patients at three California hospitals has already seen two of her colleagues infected with the virus. The scarcity of protective gear at work is still so bad that she’s wearing N-95 masks that she found from Craigslist.
She’s isolating from her family out of fear she could sicken her loved ones and now she’s unlikely to make her $4,000 monthly medical school loan payments.
DOCTORS IN DISTRESS, QUARANTINE SEND SOS FOR MORE PROTECTIVE GEAR, TESTS: ‘IT’S A COMPLETE MESS’
“When the military gets sent out to a war zone, they get hazard pay for that,” the doctor told Fox News. “… We’re taking on this risk. And if you’re not going to give us hazard pay, at least don’t cut our pay. Don’t give us less for us having to take on more. It just doesn’t really make sense.”
Fox News interviewed doctors across the country dealing with pay cuts. All were scared to speak out against their employers for fear of losing their job, so Fox News agreed not to publish their names in order to tell their previously unreported stories.
The ER and urgent care doctors were from five different states and their salary ranged from about $215,000 to $260,000 before the cuts.
While their income level is clearly above the national average, the doctors said they maintain fairly modest lifestyles — “I live in a one-bedroom apartment and I drive a Honda,” one doctor said.
The pay cuts are especially hard to handle because the doctors graduated medical school with a staggering amount of debt — ranging from about $225,000 to $420,000 in student loans– and they’ve tightly budgeted for the steep monthly payments.
Morale was already low among the doctors, and anxieties were reaching a powder keg level at some COVID-19 hotspots as doctors felt undersupplied and unsafe at their jobs, according to some doctors. So the timing of the pay cuts especially infuriated frontline doctors.
“We were kicked while we were down,” said a New York emergency physician who already received a 10 percent pay cut and is expecting more.
The doctor has a $4,000 monthly student loan bill on top of her mortgage payment. She said staff at her hospital are “terrified” at work every day treating COVID-19 patients without the appropriate Personal Protective Equipment (PPE).
The job in the ER now is “absolutely more dangerous,” the doctor told Fox News. “It’s definitely more labor-intensive and it’s just harder work. We’re all in there every day … basically terrified about what’s going to happen.”

A patient is wheeled out of Elmhurst Hospital Center to a waiting ambulance, Tuesday, April 7, 2020, in the Queens borough of New York, during the current coronavirus outbreak. New York Gov. Andrew Cuomo said last week that as city hospitals fill up, some patients could be moved to other facilities in the state to ease the crunch on local medical centers. (AP Photo/Kathy Willens) (AP)
The conditions mean that doctors are awaiting the day when they become infected.
“Every week, when you’re going back to your shifts, you’re just waiting for that fever [to hit you] … So the stress is just eating you alive,” the New York ER doctor told Fox News. “Then, you’re told you’re not worth what you once were worth when you’re doing more and working harder. It’s just sort of disheartening.”
While there is incomplete data nationwide on how many health care workers have contracted COVID-19 in the United States, Buzzfeed News confirmed at least 5,400 infections from states willing to provide data and at least 30 deaths.
New York Dr. Frank Gabrin, who raised concerns about the lack of protective gear, became the first American ER doctor to die from COVID-19 on March 31.
Emergency rooms and intensive care units around the country are the battlegrounds for the deadly pandemic but despite their outsized importance, hospitals say they are actually losing money during the pandemic, which has forced them to cut pay, reduce hours and layoff employees.
Elective surgeries at hospitals have been shelved. Patients are scared to seek care for fear of catching COVID-19. Stay-home guidelines mean there’s less chance for routine injuries from sports, car crashes, drunken bar fights, and other traumas.
Patient volume in emergency rooms, alone, has decreased by about 30 percent nationwide since the COVID-19 pandemic began, according to the American College of Emergency Physicians.
Aside from the reduction in accidents and injuries from quarantines, patients are also delaying care for fear of contacting the coronavirus while in the hospital, the group said in an April 3 letter to Health and Human Services Secretary Alex Azar seeking $3.6 billion in emergency funds.
@emergencyDocs@EmergencyDocs
Coping with sickness and stress https://www.aamc.org/news-insights/coping-sickness-and-stress … #HealthCareHeroesCoping with sickness and stress | AAMCClinicians across the country are dealing with stark increases in COVID-19 infections and anxiety. The emotional and physical toll on them is only beginning.
The American Hospital Association, a group that represents nearly 5,000 hospitals and other health care providers, has been sounding the alarm to Washington for more help and acknowledged layoffs and furloughs at hospitals throughout the country and “inadequate” PPE.
“Unfortunately, like other sectors across the nation, hospitals and health systems have experienced an economic decline due to the COVID-19 pandemic,” an AHA spokesperson said in a statement to Fox News. “This strain has resulted in some hospitals having to furlough or layoff health care workers to respond to this public health crisis. Lost revenue is due in large part to the cancellation of elective surgeries and the deferral of other non-urgent treatments and visits.”
Hospitals and health care providers were allocated $100 billion in the $2.2 trillion stimulus package known as the CARES Act that President Trump signed in law last month, and Democrats are already pushing for at least $100 billion more in the next phase of coronavirus relief.
TRUMP SIGNS $2T STIMULUS BILL AFTER HOUSE APPROVES HISTORIC CORONAVIRUS RESPONSE
“Quickly making funds available from the CARES Act will help hospitals and health systems continue to put the health and safety of patients and personnel first, and in many cases, may actually ensure they are able to keep their doors open,” the AHA said. “We are also supportive of bonus pay for front-line workers during the pandemic.”
The hospital association acknowledged their doctors are anxious about protecting themselves from the contagious new virus and called on President Trump to fully use the Defense Production Act to increase the production of PPE and medical supplies they are currently lacking.
SENATE DEMS CALL FOR ‘HAZARD PAY’ FUND
There are efforts underway in Washington to reward front line workers financially for their sacrifices. Senate Democrats have proposed a new “heroes” fund to assist health care professionals and other essential workers, like grocery store employees, with bonus pay for up to $25,000 this year. A GOP proposal in the House, led by Rep. Bill Huizenga, R-Mich., would give health care workers and first responders a federal tax holiday.
But it’s unclear, when or if, relief will come. In the meantime, non-front line doctors are even worse off. Dermatologists, podiatrists, and other specialists have shut down their offices and had to furlough their staffs as non-essential activities have ground to a halt around the country during the pandemic.
The New York ER doctor treating COVID-19 patients with reduced pay and inadequate supplies said she actually feels worse for her specialist friends. They still have to pay their student loans, medical malpractice insurance, and business operations with even less money coming in.
“Even though I took a 10 percent hit, some of them are taking like an 80 percent hit,” she said.
Front-line doctors say when they delivered their pay cut news to friends and family they were met with degrees of shock. How could doctors get less pay when their jobs have never been riskier and seemingly never more valued?
“Every person I’ve told has been astonished,” said one general practitioner who works at an urgent care clinic in Texas. The clinic only has N95 masks because she got a donation personally and shared them with the company.
The doctor got an email this month from her company that salaries were cut 10 percent across the board and all their paid time off — ranging from two to three weeks — “was just taken away.”
“Everybody assumes that doctors are wealthy people but most of us aren’t,” said the doctor, who rents a one-bedroom apartment.
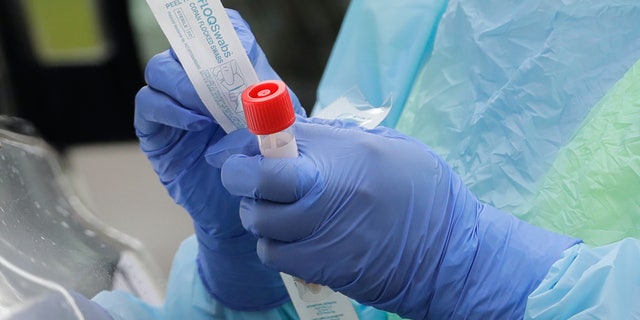
In this April 2, 2020, file photo a nurse holds a vial and a swab at a drive-up coronavirus testing station at a hospital in Seattle. A federal report out Monday, April 6, finds that three out of four U.S. hospitals surveyed are already treating patients with confirmed or suspected COVID-19. (AP Photo/Ted S. Warren, File)
The Urgent Care Association, a group that represents more than 3,300 health clinics, attributed pay cuts directly to a severe loss in caseload due to COVID-19. Revenue at most urgent care clinics nationwide plummeted 50 percent during the pandemic, according to the association.
“Urgent care is on-demand, walk-in health care,” Laurel Stoimenoff, CEO of the Urgent Care Association, said in a statement to Fox News.
Patients were getting “mixed messages” on whether they should go to urgent care for COVID-19 symptoms over concerns of spreading the virus to urgent care staff that lacked proper PPE. Patients were also told to shelter at home and use telemedicine, Stoimenoff said.
“All of these factors created a perfect storm and unfortunately, patients ceased seeking care externally by a significant percentage. …. When income is cut in half, it is difficult to maintain the same expense levels,” Stoimenoff said.
An FDNY medical worker wears personal protective equipment outside a COVID-19 testing site at Elmhurst Hospital Center, Wednesday, March 25, 2020, in New York. (AP Photo/John Minchillo)
As a result, urgent care operators around the country are making tough choices on how “mitigate the impact of this unprecedented situation” while trying to preserve health care access in the community.
“Some are cutting hours while others with multiple sites are consolidating services into certain sites while closing others. All these efforts ultimately affect payroll,” Stoimenoff said. “The goal is to be able to again open their doors when we return to a new normal.”
The massive CARES Act signed into law in March includes $350 billion for small businesses to apply for up to $10 million in forgivable loans to cover payroll costs for two months. The program, known as the Payroll Protection Program, is “a start,” Stoimenoff said.
But provisions in the legislation that exclude independent contractor wages and cap employee wages at $100,000 disadvantage urgent care operators from getting enough aid to cover payroll, Stoimenoff said. Federal changes to the aid program are needed to better help urgent care employees and clinicians who are on the front line risking their own health.
“They need help and they need it now,” she said.
DEMS BLOCK MCCONNELL BID TO SWIFTLY APPROVE $250B MORE FOR SMALL BUSINESS FUND
The Payroll Protection Program has already been inundated with applications, prompting Treasury Secretary Steven Mnuchin to request Congress pass an additional $250 billion immediately before the fund dries up. The effort failed in the Senate on Thursday and it’s unclear when lawmakers can overcome the impasse.
At a time when their jobs have become riskier and more stressful than ever, doctors say the blow to their income has shaken them with new financial anxieties. Doctors interviewed by Fox News doubted they could manage hefty student loan payments and housing costs, while others have already pared back any non-essential spending, retirement 401(k) plans, and children’s college savings.
The financial hit comes at a time when doctors said their years of education and practice already felt undervalued, especially with the rapid growth of nurse practitioners that are cheaper than doctors to employ.
“Morale among doctors is very low,” said one Texas physician. “I don’t feel like I’m respected at all. I feel like the general public values nurses much more than doctors now in this country. I think that they believe they can get whatever knowledge I have in my head from Google.”
To add insult to injury, New York doctors are being asked to leave their jobs to take “unpaid volunteer positions” at COVID-19 hotspot hospitals, like Elmhurst Hospital in Queens, Lincoln Hospital in the Bronx and Woodhull Hospital in Brooklyn, according to an email from NYC Health + Hospitals viewed by Fox News.
Meanwhile, nurses are being recruited to come to the epicenter of the outbreak with lucrative offers of $10,000 per week, plus additional money for travel, food, and lodging, according to a Facebook ad posted by a nurse recruiter for NYC Health + Hospitals.
NYC Health + Hospitals, the largest public health care system in the nation, did not respond to Fox News’ request for comment on the disparity, but doctors weren’t happy.
“It was very upsetting. It almost seemed physician altruism was being manipulated by hospital systems,” said one Manhattan physician who has received many “volunteer” requests. “It also made it seem like a physician’s life was not worth as much. It would be one thing if they asked everyone to be volunteers, but that’s not the case.”
The pay structure for doctors is complicated. Medical facilities can employ doctors directly or through contracting agencies. Doctors can be salaried, but the physicians interviewed by Fox News largely were paid either hourly or by “relative value units (RVU)” or a combination of both.
RVUs are an imperfect way to calculate physicians’ productively. The more patients a doctor sees, the more RVUs they generate. The more RVUs they generate, the more money they get paid.
Since the overall caseload is down in many emergency rooms, doctors are seeing fewer patients, which means they are generating fewer RVUs during their shifts.
Coronavirus cases are much more labor and time-intensive, especially given the effort to suit up with protective gear and properly take it off afterward treating the patient.
“I can probably take care of five to 10 finger dislocations in the amount of time it takes for me to take care of one patient who has COVID,” said one emergency physician in Virginia, whose roughly 15 percent pay cut came in the form of fewer hours and RVUs generated.
With stay-at-home orders in place, the caseload in his emergency room is down. But the patients that do come, tend to be much sicker. Yet the current pay structure doesn’t reward doctors for the harder work– just the opposite, the doctor said.
“In general, the RVUs generated for people that are very sick tend to be lower than RVUs for other quicker things, because of the amount of time involved,” the doctor explained to Fox News.
Envision Healthcare@EnvisionLeads
Envision Healthcare announced today its strategy to support clinicians fighting on the front lines of the COVID-19 pandemic and ensure we can continue to care for patients and communities once the crisis has passed. Read our full statement here: https://bit.ly/39UiREs 2
Meanwhile, hospitals and staffing companies throughout the country continue to announce major cutbacks to doctors’ pay.
Envision Healthcare, which has 27,000 clinicians nationwide, announced Wednesday doctors’ pay will be cut in areas with lower patient volumes.
Jim Rechtin, President and CEO of Envision Healthcare, said COVID-19 has “fundamentally destabilized” the health care sector. The company is also temporarily suspending retirement contributions, bonus pay and promotions. Senior executives will get a 50 percent pay cut and nonclinical staff will have salary reductions and temporary furloughs.
Alteon Health, a medical staffing company with 1,700 clinicians, had planned for 20 percent cuts to medical director stipends and suspending 401(k) matches, bonuses and paid time off, ProPublica first reported March 31. While the large emergency room employer reversed some of the cuts after they were reported, Alteon still intends to convert salaried employees to hourly and reducing hours of clinicians in certain hospitals –which has the effect of a pay cut, the news site reported.
Atrius Health✔@atriushealth
To protect the health of our patients & staff, we have temporarily suspended some of our practice operations and made changes to our walk-in lab, pharmacy, and optical shop operations. Please continue to call your doctor’s office for medical advice & care http://ow.ly/xXxx50z3GVw Coronavirus Disease (COVID-19) InformationAtrius Health is closely monitoring the international spread of coronavirus disease (COVID-19) and we want to do all we can to help our community stay safe and healthy.atriushealth.org
Atrius Health, Massachusetts’ largest independent physician network, experienced at least a 70 percent drop in patient visits since hospitals and clinics began canceling elective surgeries, procedures, and office visits. As a result, some employees are on a one-month furlough and those doctors and nurses still working will have on average 20 percent or their pay temporarily withheld, WBUR Boston reported.
Doctors say their anxieties over treating COVID-19 patients and their new financial strains are especially tough to cope with when they are purposely isolating themselves from loved ones they fear infecting with the deadly virus.
“You’re dealing with the stress at work. You don’t feel safe at work,” the Los Angeles doctor told Fox News. “And now you’re alone when you go home and you don’t even have anybody there that you can really lean on for support.”






